How to prevent suicide
Said Shahtahmasebi, PhD.
The Good Life Research Centre Trust. Email: radisolevoo@gmail.com
Key words: suicide; suicide prevention; public health; grassroots; depoliticising
Received: 2/11/2017; modified: 16/11/2017: accepted: 22/11/2017
Abstract
Recent suicide figures for 2017 released by the chief coroner’s office showed that suicide in New Zealand has reached a record high for three years running. With signs of despair the government has promised an increased investment in the mental illness services. But this is what they did over the last three years and the years before, and every time suicide data has been released. Finally, the mainstream media reported an admission by a psychiatrist what most of us knew already that nothing works in reducing the suicide rate. But this admission is false and should have stated that nothing that psychiatrists do works in reducing the suicide rate. This paper identifies the problems associated with the current suicide prevention strategy of medicalising suicide, and offers an approach that is effective.
Introduction
Figures released by the New Zealand Chief Coroner’s Office (Shahtahmasebi, 2017a)showing a sharp increase in suicide numbers for three years consecutively have shocked the ‘experts’ and public. At last someone finally has admitted that there is a problem; the mainstream media published an admission with the headline “psychiatrist warns that ‘nothing’ is working in bid to address suicide rates” (Stuff.co.nz, 2017). Surely the headline meant that nothing ‘medical’ is working.
The medicalisation of suicide presumes illness of the mind from the outset and in this context throughout the remainder of this paper the unconventional phrase ‘mental illness’ services is used instead of the conventional mental health services.
To solve a problem we must have a good understanding of what the problem is — suicide prevention is no different.
We literally have no idea or understanding of suicide and why some people choose death over life. But we do have a better understanding of human behaviour. So it is reasonable to assume that we can reduce or stop all suicide by targeting behaviour.
However, to achieve a successful suicide prevention action plan we must first consider the issues that have arisen from the established suicide prevention strategies which assume that suicide is the outcome of a mental illness.
Problem 1 – Intervention as a suicide prevention strategy
- Globally there is one universal ‘mental illness’ approach to suicide prevention
- The mental illness approach confuses prevention with intervention i.e. the model promises to prevent suicide through psychiatric intervention.
- This model allows the inevitable to occur (suicidality), which in the context of prevention is far too late, and then attempts to stop suicidality through the use of medication.
- Whereas prevention means changing the behavioural processes so that suicidality is removed.
- Even as an intervention psychiatry is ineffective for the following reasons:
- Between two-thirds and three-quarters of all suicide cases do not come into contact with mental illness services.
- In other words, between one-quarter and one-third of all suicide cases do come into contact with mental illness services – and yet they go on to complete suicide.
- These statistics suggest that psychiatry is not equipped to intervene and stop suicide.
- Case studies reveal that suicide cases are regarded as mentally ill thus a need for a psychiatric diagnosis for which medication can be prescribed. (Shahtahmasebi & Smith, 2013)
- Furthermore, there is strong evidence that medications such as antidepressants can be responsible for suicidality and completed suicides. (Khan et al., 2000)
Thus, with attention firmly focused on diagnosing and treating a mental illness suicide per se is removed from any intervention plan.
Problem 2 – flogging a dead horse
Hence tax-payers money has been poured into mental health services to support an interventional scheme which has never worked and does not produce tangible results and gives the public more of the same each year. For decades with more resources, more mental illness services are promised, and with more mental illness services fewer suicides are promised. In other words, ‘more of the same’ is the whip that is flogging the dead horse. This is a political manoeuvre: by announcing the investment of ‘additional’ resources in mental health services, governments around the world firstly keep the public at bay by stating that they are combatting the suicide problem, and secondly keep psychiatrists happy. But is this enough?
For decades, suicide has been confused with mental illness and as such the official suicide ‘prevention’ guidelines made available to the public has been to look for signs of mental illness and refer to mental health services for help. This is a ‘comedy of errors’: if signs of suicidality are detected then our prevention plans have failed and it is time to intervene to stop suicide.
The only outcome of this suicide prevention policy is that the authorities and experts claim downturns in the suicide rate as their own success but refuse to take responsibility for the upturns in suicides.
Problem 3 – policy of secrecy and silence
To prevent the public wising up to the ‘more of the same’ strategy, the authorities and ‘experts’, notably in New Zealand, have come up with a policy of silence around suicide. This strategy and the claim that it will reduce suicide (and copy cats) has been challenged and dismissed (Shahtahmasebi, 2014b), however, the implications of such a policy is public ignorance about suicide leading to loss of lives.
If public discussions about suicide are allowed along with appropriate and relevant quality information members of the public are in a position to hold a conversation with someone who is feeling suicidal instead of turning away in the hope that someone else may intervene.
There are many problems with such strategies as it reduces the chance of a suicidal individual sharing his/her feelings with someone else for fear of being misunderstood, fearing being labelled, and being sectioned. An educated public encourages ‘feelings’ to be articulated and shared without prejudice. Under the policy of silence the public’s contribution is to look for signs of depression and refer to mental illness units.
Another adverse outcome of a policy of silence is the mystification of suicide especially amongst adolescents who have been known to glorify suicide, and spread inaccurate information about suicide to their peers (Omar, 2013).
Problem 4 – Patterns in suicide rates
Suicide rates often demonstrate a cyclic pattern (Shahtahmasebi, 2017b) which can only be observed over a long period of time. The biggest mistake made frequently by decision makers and planners is to compare the current suicide rate with that of the immediate preceding year(s). If the rate for the current year is lower (regardless of previous patterns) credit is claimed by the authorities and ‘experts’ for reducing the rates and when it is higher than the previous year no responsibility is taken thus they claim that suicide is a complex social and economic issue!
It may be public apathy that three years in a row suicide numbers have hit a record high (Shahtahmasebi, 2017a). All that has been offered by the government is more investment in mental health services to provide ‘more of the same’ at a very high cost.
As shown in Figure 1 there are many cycles of varying length. The current patterns in suicide rates were predicted in 2001 but the New Zealand government ignored ‘suicide’ and instead invested in mental illness services. For example, in publishing its 2006 suicide prevention strategy citing social, health, economic and mental illness as suicide risk factors, the New Zealand government failed to lead a new direction and instead diverted funding to tackling depression as its action plan for preventing suicide (Shahtahmasebi & Shahtahmasebi, 2010)!
When conflicting trends (e.g. male vs female, or by age group) are plotted an important observation is made that should influence the policy development process. Notably there is a lagging effect between each group. That is to say the trend for females on average is behind by several years, i.e. when the trend for men is downward the trend for females is upward. A similar lagging effect can be observed for other groups such as age, occupation, etc.
A mistake frequently made by the ‘experts’ is not to recognise the lagging effect in different group’s suicide rates that basically following the same trend. For example, when the overall suicide rate is down compared with the previous year, the authorities claim success but also claim that the same policies must be enforced on groups still showing an upward trend. Thus, mistaking lags as between groups differences in suicide rates (Shahtahmasebi, 2013; Shahtahmasebi & Merrick, 2014).
The reverse is also true. When the overall suicide rate is higher than the previous year with all groups completing a full cycle, due to the lagging effect the same groups who previously showed higher rates of suicide would then show a decreasing trend, the authorities would claim credit for reducing suicide rates in these groups (Shahtahmasebi, 2013; Shahtahmasebi & Merrick, 2014).
Figure 1. Cyclic patterns in suicide trend in New Zealand
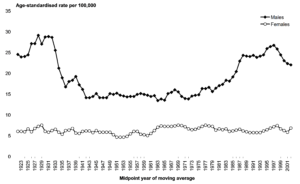
Problem 5 – academic media
While prominent psychiatric journals have ‘owned’ the suicide problem they are only interested in a discussion of medicalised suicide (Shahtahmasebi, 2014a). Unfortunately, it is the influence of such journals and research that governments tend to rely on.
As an experiment in 2013/14 a paper (Shahtahmasebi, 2014b) highlighting and critiquing two myths most commonly referred to as facts in suicide research and suicide prevention was submitted to several top journals in the fields of psychiatry and suicidology. The response from the journals was swift and similar. They politely cited a large number of submissions as their reason for not reviewing the paper and for prioritising only certain types of research, e.g. longitudinal studies, systematic reviews or meta-analysis. A quick exploration of the journals Table of Contents for the previous twelve months indicated the same old theme of depression/mental illness and suicide. Clearly by adopting such an editorial strategy the editors were contributing to the problem and indeed had become part of the problem.
Problem 6 – corporate media
Similarly, the mainstream media is fearful of discussing suicide outside of the mental illness framework. In rare cases of reporting non-medical suicide prevention initiatives they focus their reporting within the medical model, or edit out the report altogether! For example, in order to help open up a public discussion of suicide the media reports either the coroner’s findings or a suicide case but always associates the suicides with mental illness (Shahtahmasebi, 2005; Shahtahmasebi & Merrick, 2014), and demands more investments in the mental illness services, and finishes off by listing telephone numbers where to get help if feeling depressed or suicidal.
A common perception, at least in theory, is that journalist codes of ethics dictate the search for ‘truth’ by reporting on all sides of the issue. It is not clear why the media sees its behaviour as being in the public interest.
Problem 7 – ‘experts’ and politicians
In 2014/15 in New Zealand, the Government’s response to a record number of suicides was to invest more in the mental illness services. No questions asked.
In 2015/16 the Government’s response to record number of suicides for the second year running was to strengthen mental illness services, and invested more in mental illness services (Shahtahmasebi, 2016). No questions asked.
In 2016/17 the Government’s response to record high suicide numbers for the third year running was to strengthen mental illness services, and promised to invest more (Shahtahmasebi, 2017a). No questions asked.
For decades, the ‘experts’ have convincingly claimed that suicide is caused by mental illness, this is despite psychiatric units own data rebuking such a claim. Nevertheless, the ‘experts’ have somehow convinced the public at large of a link that doesn’t exist, and persuaded the decision makers that tackling mental illness is the only way to prevent suicide. Thus psychiatry has owned the suicide problem.
This approach has created a top-down culture that excludes the public, the real stakeholders, from taking part in defining the problem and finding a solution. In other words, the ‘experts’ know best and all the public can do is to look for signs of depression and refer to mental illness units. As the evidence has shown this approach has failed to break the cycles in suicide rate trend and failed to reduce the numbers of suicide leading to record number of lives being lost to suicide.
Typically this has been the Government’s and ‘experts’ response to suicide numbers (whether high or low) for decades. In any other business the funders would be demanding an explanation (and resignations and new directions for action) as to why the service has not delivered.
As things are, governments, researchers, and ‘experts’ are all part of the suicide problem. For example, zero suicide was reported for Christchurch (NZ) following the 2010/11Canterbury earthquakes. The ‘experts’ warned that suicide rates post-earthquake would increase. Instead of proactively developing health, social and financial support initiatives, the government and the ‘experts’ sat on their hands waiting for signs of suicide to develop. Canterbury now boasts the highest suicide rate in New Zealand (Shahtahmasebi, 2017a).
Problem 8 – the public
Suicide is a taboo subject and with the policy of silence this status has been strengthened. It is often easier to let the medical professionals deal with illness and death. Therefore, the public at large is often vague about how to deal with someone who may be feeling suicidal and therefore reluctant to engage with them. As mentioned above (problem 1) between three-quarters and two-thirds of all suicides do not contact health services and die in isolation, and the other quarter/third who do receive help still go ahead and complete suicide also in isolation.
Our perceptions and how we behave towards suicide has therefore made us part of the suicide problem, too.
Problem 9 – knowledge and suicide training
While the public reaction to suicidality can, in part, be blamed on the taboo status of suicide and the government’s mental health policies, the main issue here is a lack of knowledge and quality information about suicide. There is anecdotal evidence that suggests those who complete suicide have tried to tell someone how they feel but we frequently misinterpret or do not hear them (Omar, 2013).
As mentioned above, due to a policy of silence, there is very little or no quality information or training available in the public domain.
For some time now a number of myths about suicide has been dispelled, in particular the link with mental illness (e.g. see (Hjelmeland et al., 2012; Shahtahmasebi, 2014b; WHO, 2014). But unfortunately, as mentioned above the corporate and academic media have failed to publicise these in the same way they publicise that depression is a major risk factor for suicide!
How to reduce suicide:
1. Throwing out the key with the lock
For many decades mental illness has been used as the key to understand suicide and unlock its mystery in order to prevent it. Clearly, the evidence (e.g. the record high suicide numbers three years in a row 2015-17 (Shahtahmasebi, 2017a) very strongly demonstrates that the mental illness approach is the wrong key to unlocking suicide. The problem with suicide is that it has become much more complex due to decades of forcing the wrong key into the wrong lock. In other words both the lock and key have been heavily damaged to such an extent that the key is stuck or broken inside the lock, thus preventing us from trying other keys.
Fortunately, because the key (mental illness) has been used to define the lock (suicide) it is possible to throw away the broken key and lock and start afresh.
We do not understand suicide per se. As the evidence of the past decades show— suicide is not caused by mental illness, nor is it caused by bereavement, stress, relationship break ups, unemployment, specific occupations (farmer, pilot, accountant, etc.), skin disease, cancer, being a student, turbulent childhoods, disability, hardship, youth, middle age, and so on. However, a small proportion in each of the above groups does complete suicide. In other words, everyone is at risk of suicide. So it is the public that holds both the key and the lock to suicide prevention, i.e. we can no longer view suicide as mental illness.
2. Stake-holders (key-holders)
Current suicide strategies around the world are top-down and the problem of suicide is exclusively owned by the ‘experts’ and decision makers, i.e. unless one is a psychiatrist or psychologist one cannot reasonably make any comments about suicide and its prevention.
Given the evidence of the last few decades the ‘experts’ and decision makers seem to be far removed from the realities of suicide and have actually made the problem much more complex.
The upshot is that mental ‘health’ services are in disarray, the public is fearful of suicide and therefore lacks the knowledge and relevant information to engage with a suicidal person, suicide survivors are ignored and left unsupported, and the suicide rate is still trending upward. In October 2017 the media reported a psychiatrist’s warning that ‘nothing’ is working to bring down suicide rates (Stuff.co.nz, 2017).
Of course, this statement is false and is the result of a top-down culture, and clearly demonstrates the media’s poor behaviour towards suicide prevention as discussed under problem 6.
There are local initiatives that have reduced suicide within the localities that they were developed but because they are not psychiatry-led they are dismissed as non-scientific within a culture of a top-down medicalised suicide prevention. The prevention strategies that do work are when all stakeholders, not just the one group, are empowered to be part of the solution.
In 2010, after many years of seeking collaborations across the government agencies to develop suicide prevention strategies, when it was realised that neither resources nor a change in attitude was forthcoming, the problem of suicide was taken to interested local communities. They were informed that they are the stakeholders; they know their communities better than any experts or decision makers. It is up to them to find the key and unlock the problem of suicide.
The grassroots approach
The grassroots approach to youth suicide prevention is fully discussed elsewhere (Shahtahmasebi, 2013). The point is made here that a lot can be achieved with little funding through empowering the public.
The grassroots approach is a direct reaction to a top-down culture of delivering mental care. The philosophy behind the grassroots approach came about because no one at the top was willing to do something for those at the bottom and had excluded them. Then grassroots took the initiative and did something for themselves. To develop their own initiatives grassroots must have information, so that they can talk about suicide and articulate issues relevant to them.
We do not understand suicide. It is unwise to claim otherwise especially in view of the decades of accumulating evidence showing that mental illness has nothing to do with suicide. Stakeholders at grassroots level need real and relevant information. From a practical standpoint, suicide is a human behaviour outcome, and we understand more about human behaviour than suicide. So, equipping the grassroots with information on adolescent development and human behaviour will empower them to develop local initiatives to prevent suicide.
In New Zealand between 2010 and 2015 training workshops were offered to communities free of charge and made available to members of the public (Shahtahmasebi, 2013). The information obtained from the workshops was taken back to the communities and grassroots suicide prevention groups were established with the task of mobilising the community, using locally developed initiatives, to help prevent suicide. Youth suicide numbers dropped considerably and still remain low in the communities that took part (Brown, 2016; Shahtahmasebi, 2013; Shahtahmasebi & Smith, 2013).
References
Brown, J. (2016). Grassroots suicide prevention in a youth education setting – update. Dynamics of Human Health (DHH), 3(2), http://www.journalofhealth.co.nz/wp-content/uploads/2016/2006/DHH_Brown_YMCA-Update.pdf.
Hjelmeland, H., Dieserud, G., Dyregrov, K., Knizek, B. L., & Leenaars, A. A. (2012). Psychological autopsy studies as diagnostic tools: Are they methodologically flawed? Death Studies, 36(7), 605-626.
Khan, A., Warner, H. A., & Brown, W. A. (2000). Symptom reduction and suicide risk in patients treated with placebo in antidepressant clinical trials: An analysis of the food and drug administration database. Arch Gen Psychiatry, 57, 311-317.
Omar, H. (2013). Understanding adolescents. Suicide prevention at grassroots workshops, Hamilton, New Zealand.
Shahtahmasebi, S. (2005). Suicides in new zealand. ScientificWorldJournal, 5, 527-534.
Shahtahmasebi, S. (2013). De-politicizing youth suicide prevention. Front. Pediatr, 1(8), http://journal.frontiersin.org/article/10.3389/fped.2013.00008/abstract.
Shahtahmasebi, S. (2014a). Problems with interpreting and reporting suicide research. Dynamics of Human Behaviour, 1(4), http://www.journalofhealth.co.nz/wp-content/uploads/2014/12/DHH_Said_Problems.pdfhttp://www.journalofhealth.co.nz/wp-content/uploads/2014/2012/DHH_Said_Problems.pdf.
Shahtahmasebi, S. (2014b). Suicide research: Problems with interpreting results. British Journal of Medicine and Medical Research, 5(9), 1147-1157.
Shahtahmasebi, S. (2016). Suicide prevention: Politics or conspiracy. Dynamics of Human Behaviour (DHH), 3(4), http://www.journalofhealth.co.nz/wp-content/uploads/2016/2012/DHH_Said_Suicide-on-the-rise.pdf.
Shahtahmasebi, S. (2017a). Editorial: Suicide numbers a record high for the third year running. Dynamics of human health (DHH), 4(3), http://www.journalofhealth.co.nz/?page_id=1160.
Shahtahmasebi, S. (2017b). A working model of suicide prevention. Dynamics of Human Behaviour (DHH), 4(1), http://www.journalofhealth.co.nz/?page_id=750.
Shahtahmasebi, S., & Merrick, J. (2014). Suicide from a public health perspective. New York: Nova.
Shahtahmasebi, S., & Shahtahmasebi, R. (2010). A holistic view of suicide: Social change and education and training. Journal of Alternative Medicine Research, 2(1), 115-128.
Shahtahmasebi, S., & Smith, L. (2013). Has the time come for mental health services to give up control? J Altern Med Res, 6(1), 9-17.
Stuff.co.nz. (2017). Psychiatrists warn that ‘nothing’ is working in bid to address suicide rates. http://www.Stuff.co.nz/national/health/96946527/canterbury-suicide-rate-worrying-psychiatrist-warns-nothing-is-working?cid=facebook.post.96946527.
WHO. (2014). Preventing suicide: A global imperative. http://www.who.int/mental_health/suicide-prevention/world_report_2014/en/.